At a time when regulation in general and European regulations in particular are an easy target for derision, it should be recognised that regulations underpin the health millions of European citizens.
A regulatory divorce is a possible consequence of Brexit negotiations that go seriously “hard”, and it is possible this could delay or even deny patients in the UK access to life saving medical treatments.
Industry wants to avoid this outcome. As reported in Chief.Exec.com last week, 97 per cent of UK healthcare industries want to retain European regulations which control the safety and efficacy of their products.
To understand how such regulations enable industry to prosper and patients to be safely treated, it is necessary to look behind the scenes into how health technologies reach the clinics and the patients.
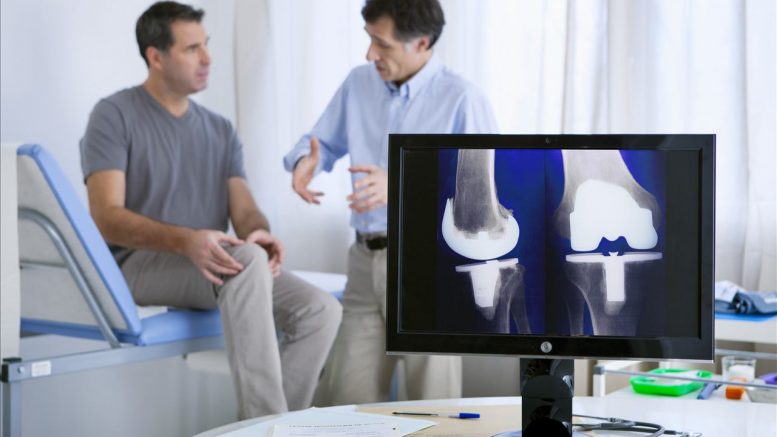
European regulations for health technology essentially balance the risks patients face with the benefits they receive from clinical treatments such as the replacement of a painful knee with an artificial joint prosthesis – a highly successful procedure through which more than 100,000 UK arthritis sufferers each year have their mobility restored.
The Medicines and Healthcare products Regulatory Agency (MHRA) is the “Competent Authority” responsible for implementing the European legislation in the UK. The Competent Authority can then authorise a number of Notified Bodies, such as the British Standards Institute, to work with and audit healthcare companies to ensure they conform to the “Essential Requirements” of the regulations.
Importantly, any Competent Authority, via a Notified Body, can authorise a medical device for use anywhere in Europe through the CE-marking process. For both industry and patients this is an advantage, as it avoids the need for expensive regulatory filings in 28 small European markets and the delay that causes.
So what could happen following Brexit?
On Sunday British Prime Minister Theresa May announced that a Great Repeal Bill – intended to repeal the European Communities Act 1972 – will appear in the next Queen’s speech. This bill will cut and paste existing EU law into British law and by doing so “make the UK an independent sovereign nation that is making its own laws”, said Mrs May to the BBC. UK Parliament can then exercise its independence by deciding which laws to keep and which to change.
We can try to extrapolate the effect of this new legislation for health technologies. The MHRA will cease to have legal responsibility for European law to become a Competent Authority for new British legislation. There would then be a case for asserting an “equivalence” of the UK system to preserve a unified European approach. The MHRA may even have some associate status allowing input into future European regulations. The UK and Europe would both benefit from such collaboration.
However, there is a paradox at the heart of the proposed new legal framework. How can the MHRA discharge its health and safety responsibilities as a Competent Authority for UK legislation based on a European regulatory framework over which they have no control?
A possible outcome is a UK regulatory approach that is a pick-and mix of new European systems that have been prepared for introduction in 2016 after eight years of gestation, together with something more bespoke, perhaps concerning special exemptions or to promote research and innovation.
In a statement MHRA confirms it is taking a business as usual approach with a focus on “protecting health and improving lives”. When consulted a spokeswoman for the MHRA said, “It is too early to be able to comment on what our role will be with regard to the EU Medical Device Directive.”
The divergence of EU and UK regulatory systems in healthcare will continue to be a matter of concern to avoid the need for duplicate regulatory filing in the UK and the rest of Europe. There will be little enthusiasm in the health technology industry to invest in expensive clinical testing and regulatory filing in what is effectively a small UK market.
Patients with knee pain may put up with alternatives or delay in treatment options. Those with an abdominal aortic aneurism may have more urgent need for a device judged effective through compliance with European medical device directives.
The importance of regulations for safety and market access is not unique to the healthcare field. European regulations feature in many other sectors such as in construction, transport and energy. How the essential healthcare regulation features in deliberations and negotiations for Brexit can provide a bellwether for much of UK industry.
by John Egan